Understanding Perimenopause and Menopause

Why am I feeling this way?
If you’ve noticed changes in your sleep, mood, energy, weight, or how your body feels overall, and you’ve been told “your labs are normal” or “this is just a part of aging”—you’re not alone.
Many women experience real, sometimes disruptive changes in midlife that are often related to hormonal transitions. At Radiant Health for Women, we help women understand what may be happening during perimenopause and menopause and whether treatment could be helpful.
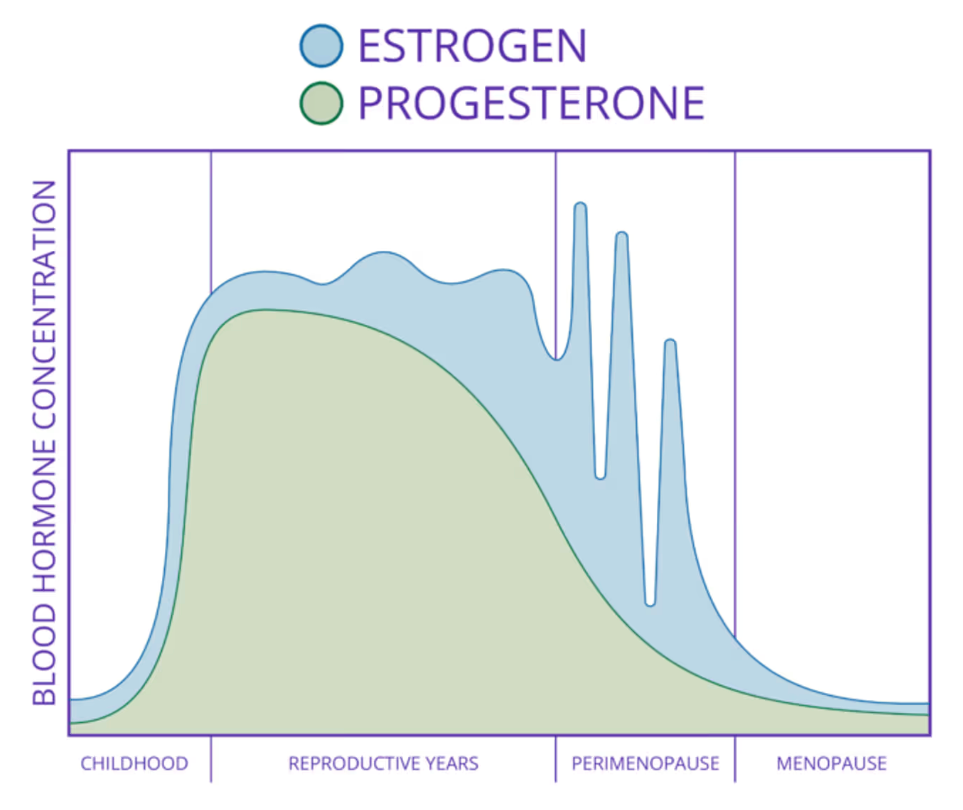
What is perimenopause and menopause?
Perimenopause is the transitional phase leading up to menopause, often beginning in the late 30s or 40s. During this time, progesterone levels decline causing estrogen levels to fluctuate wildly. This ‘estrogen roller-coaster’ can cause many changes throughout the body, even while menstrual cycles are still occurring. For many women, this is when symptoms first appear.
Menopause is defined as twelve consecutive months without a menstrual period and most commonly occurs between ages 45 and 55. At this stage, ovarian hormone production has declined more consistently, and symptoms may persist or evolve.
These transitions are a normal part of aging, but the symptoms associated with them are not something women simply have to tolerate and endure. Gaining insight into these changes is the first step toward reclaiming your agency and accessing personalized care unique to your own journey.
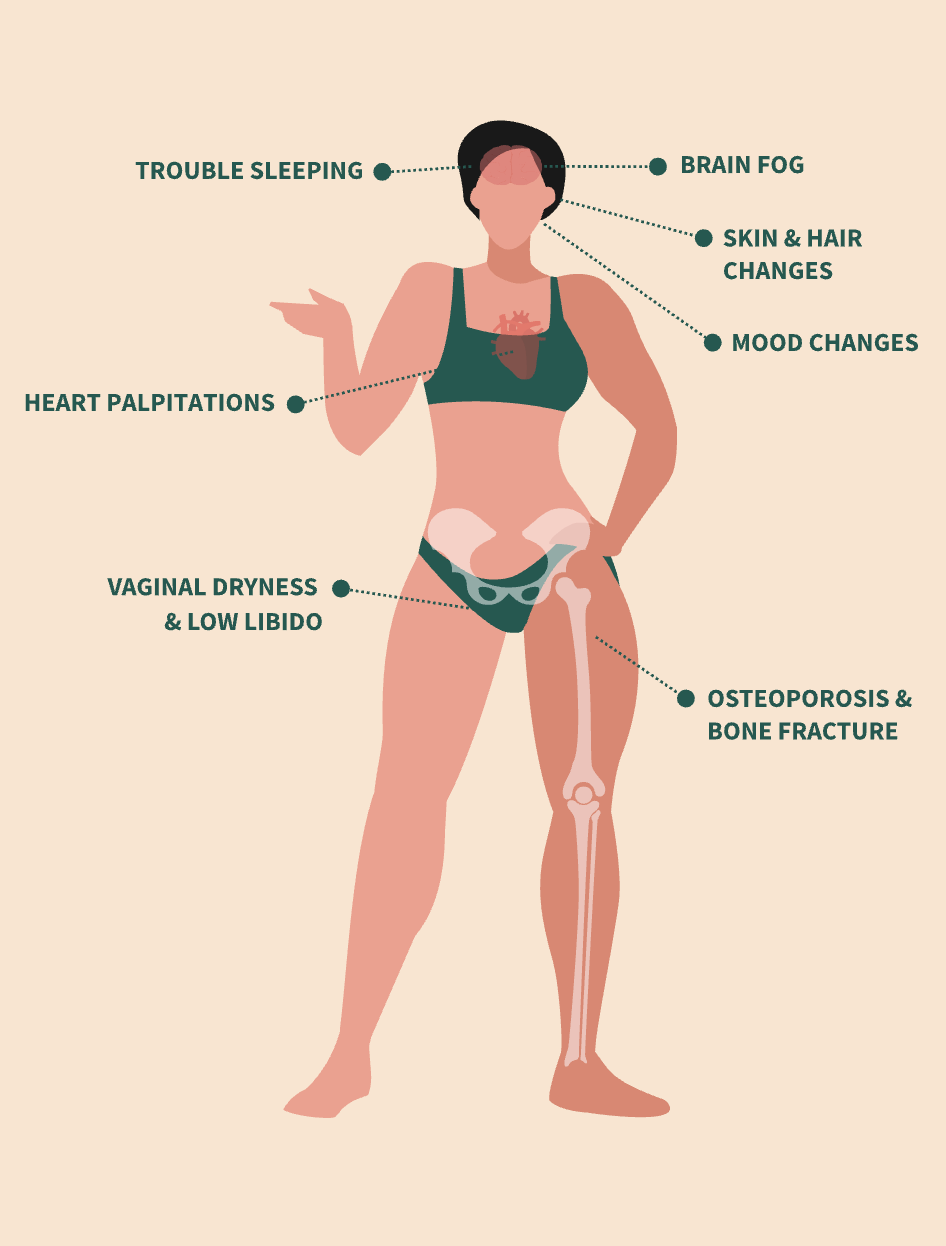
What’s happening in my body?
During perimenopause and menopause, the ovaries change how they produce three key hormones, and these hormones have an important influence on many different systems throughout the body, not just the reproductive organs:
1- Estrogen supports brain function, sleep, metabolism, bone and cardiovascular health, skin elasticity, and temperature regulation.
2- Progesterone plays an important role in calming the nervous system and supporting sleep and mood balance.
3- Testosterone contributes to energy, muscle strength, libido, and overall vitality.
Receptors for these hormones are found throughout the body, including the brain/nervous system, cardiovascular system, muscles/joints, bones, skin, metabolic tissues, and urinary/pelvic tracts—therefore hormonal changes can affect many areas all at once. Women may experience changes in:
Temperature regulation - leading to hot flashes or night sweats
Neurotransmitters - influencing mood, anxiety, focus/memory and sleep
Metabolism/Energy - contributing to weight gain, fatigue and reduced stamina
Pelvic/Urinary structure - affecting bladder and pelvic floor issues
Cardiovasular health - increased cardiovascular risk over time
Tissue health - affecting skin, hair, and vaginal comfort
Because hormone levels fluctuate (especially in perimenopause) symptoms may come and go, shift over time, or feel unrelated to one another. External factors such as stress, poor sleep, and the demands of work or family life can further amplify these effects.
Though these symptoms are grouped by when they’re most common,
they can occur at any time.
What are my symptoms?
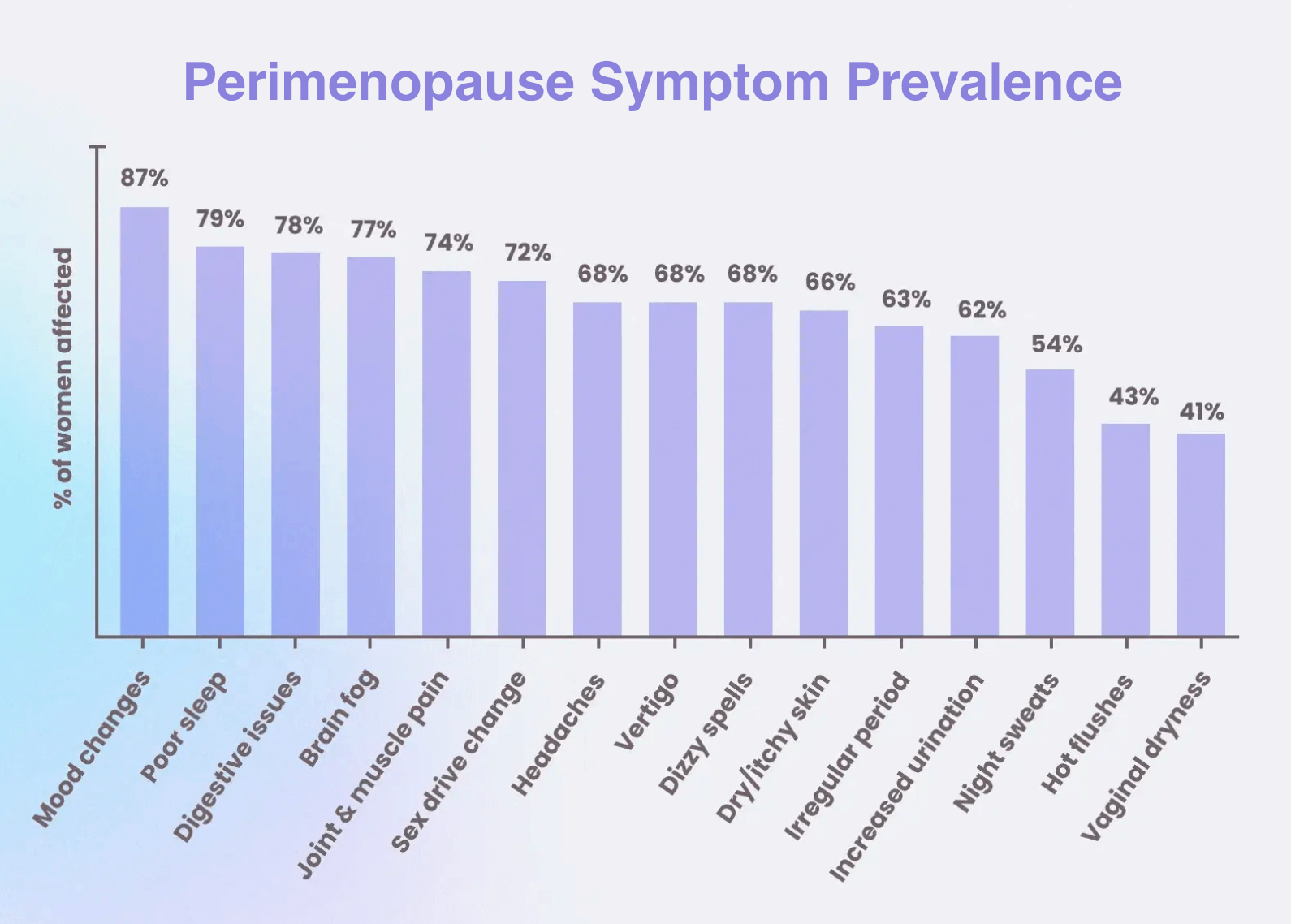
Perimenopause Symptoms
Characterized by hormonal fluctuation, not steady decline. Estrogen and progesterone levels rise and fall unpredictably, which can make symptoms feel intense, cyclical, or erratic.
Irregular, heavy, or skipped periods
Worsening PMS-like symptoms or mood changes
Increased anxiety or emotional reactivity
Weight gain or changes in body composition
Sleep disruption, especially waking during the night
Breast tenderness
Cycle-related headaches or migraines
Brain fog or difficulty concentrating
Periods of feeling well followed by sudden symptom flares
Why this happens: These changes are due to rapid hormonal swings, which can overstimulate the nervous system and disrupt sleep, mood, and cycle regulation.
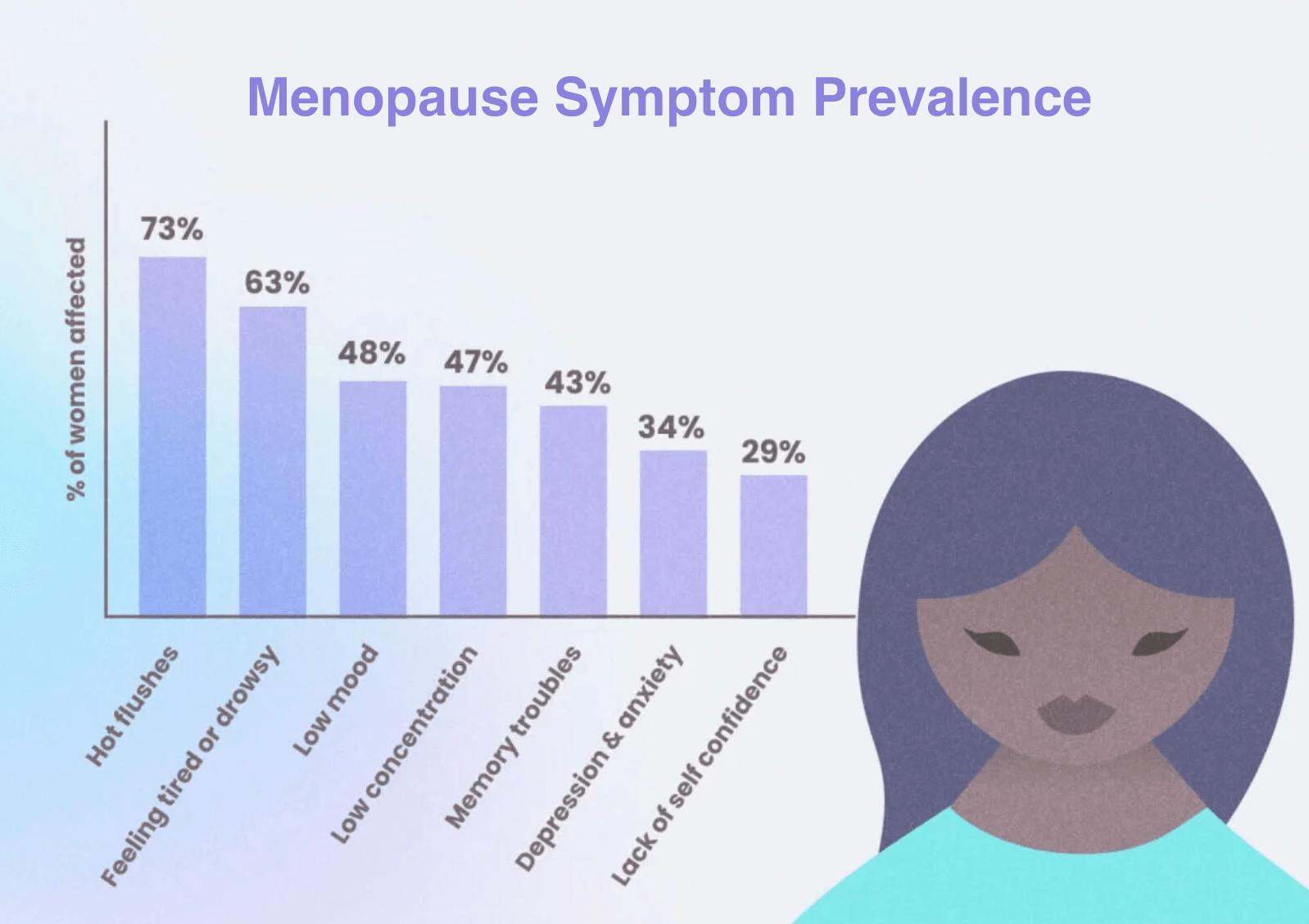
Menopause Symptoms
Menopause occurs once menstrual cycles have ended and estrogen levels remain consistently low. Symptoms tend to be more persistent.
Ongoing hot flashes or night sweats
Vaginal dryness, discomfort, or pain with intercourse
Urinary symptoms or recurrent infections
Skin thinning, dryness, or loss of elasticity
Hair thinning or texture changes
Bone density loss or changes in body composition
Joint pain and stiffness
Changes in cholesterol or cardiovascular risk
Ongoing low energy or motivation
Persistent low libido not linked to cycle changes
Why this happens: Without regular estrogen production, tissues that rely on estrogen for strength, elasticity, regulation, and repair gradually change over time.
Why are my symptoms so different from other people’s?
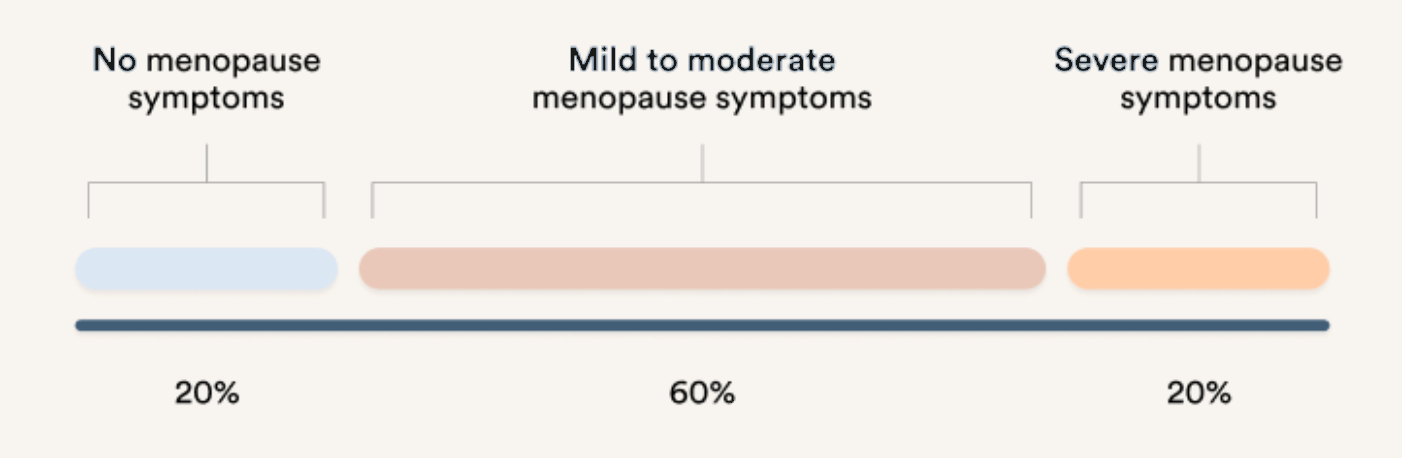
Intensity of Peri/Menopause Symptoms
experienced by women
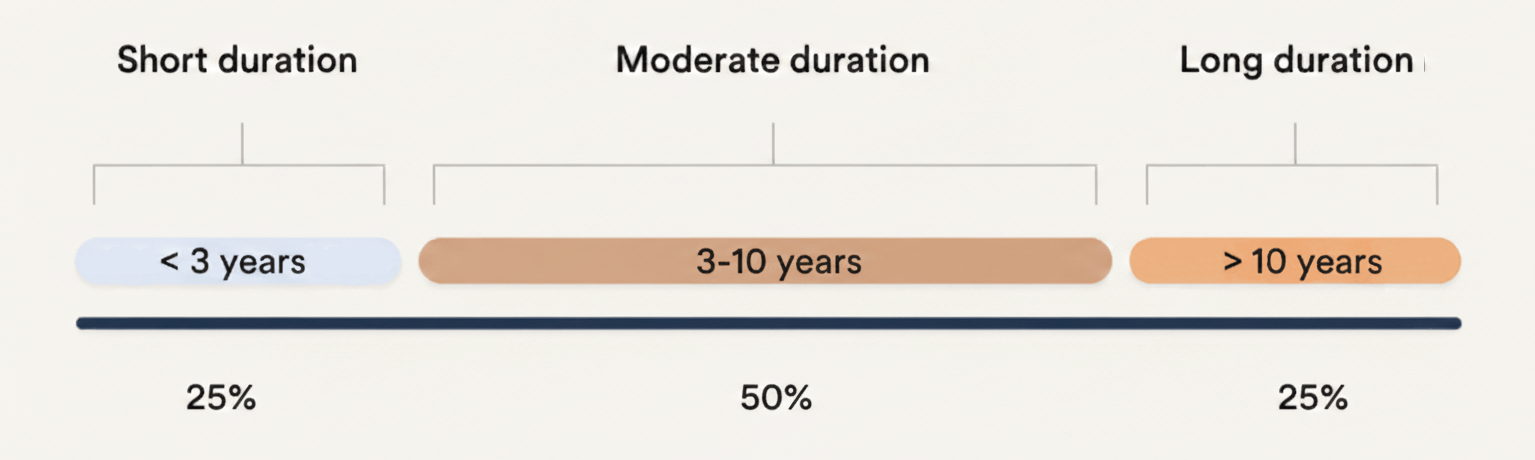
Duration of Peri/Menopause Symptoms
experienced by women
The duration and Intensity of peri/menopause symptoms that women experience differ significantly. Some have debilitating symptoms, while others have very little at all. Some experience symptoms for just a few years, while others continue to have them for over a decade. On top of this, women also experience different constellations of symptoms. One might notice sleep disruption and mood changes; while another may struggle more with joint discomfort or shifts in body composition. Why all the differences? Symptom patterns are often shaped by:
Genetics – Family trends often influence timing and severity.
Stress and life stage – Ongoing stress can amplify sleep, mood, and metabolic symptoms.
Medical history – Thyroid health, mood disorders, autoimmune conditions, and metabolic health can influence how symptoms are felt.
Past hormone exposure – Pregnancy history, contraceptive use, and reproductive patterns are linked to symptom timing and pattern set.
Lifestyle and body composition – Insulin sensitivity, muscle mass, sleep quality, and cardiovascular health influence symptom resilience.
The diverse presentations of peri/menopause women underscore the importance of finding an experienced menopause practitioner who is adept at properly assessing a patient’s condition and then administering selective treatment plans that target each patient’s unique presentation. Anyone who has symptoms that impact their quality of life can benefit from medical help. In some cases, even women with few or no symptoms may consider hormone therapy for prevention of certain diseases.
Why is perimenopause an ideal time for disease prevention?
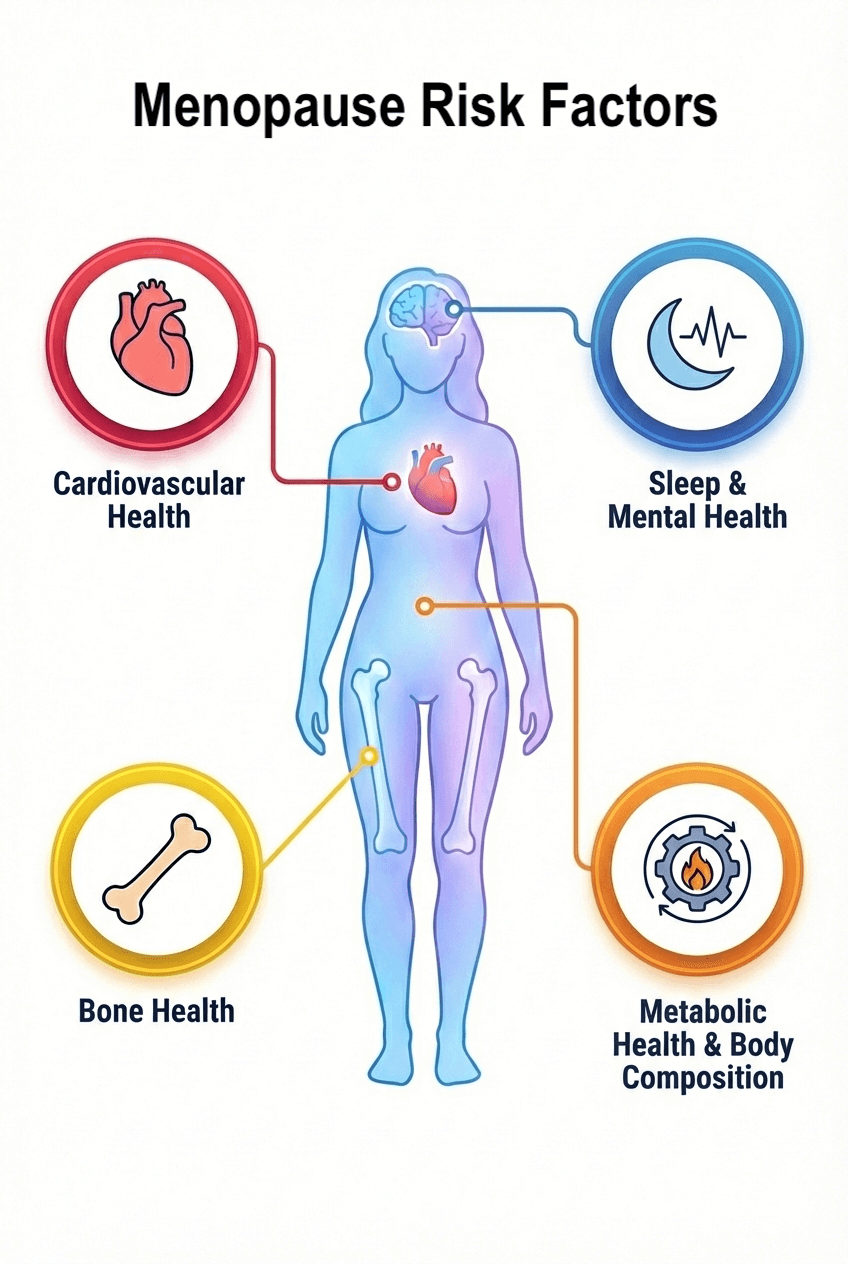
Perimenopause (and menopause to a lesser extent) represent a critical window of opportunity to protect your health for decades to come. The hormonal changes occurring during this time can affect your overall health in ways that increase your risk of future disease. Normally, your ovaries produce adequate levels of estrogen and other hormones that serve to protect multiple systems in your body. During perimenopause, as hormone levels fluctuate and decline, several critical changes start to occur:
Cardiovascular Health -the most significant long-term risk shift in midlife.
Estrogen supports cholesterol balance, and vascular elasticity and health. As levels change: LDL cholesterol may rise, blood vessels may stiffen, and blood pressure may increase. Because heart disease risk rises during menopause, perimenopause is an ideal time to assess lipids, blood pressure, inflammation, and overall cardiovascular risk—and intervene early.
Metabolic Health & Body Composition
Hormonal shifts and aging influence insulin sensitivity, muscle mass, and fat distribution. Many women notice: increased abdominal fat, loss of lean muscle, and greater difficulty maintaining weight goals. These changes are biologically driven, not simply lifestyle-related. Preserving muscle mass and improving metabolic resilience during this window can significantly reduce future risk of diabetes, cardiovascular disease, and frailty.
Bone Health
Estrogen is essential for maintaining bone density, and bone loss often begins during perimenopause, before periods have fully stopped. Without attention, this tissue loss can progress silently toward osteopenia or osteoporosis. Early strength training, nutritional support, and appropriate therapy can meaningfully alter long-term fracture risk.
Sleep & Mental Health
Hormonal fluctuations affect sleep regulation and stress response. Chronic poor sleep and stress are linked to worse outcomes for metabolic and cardiovascular health.
The advent of perimenopause presents a strategic opportunity to assess risk, build resilience, and shift from reactive care to proactive prevention—supporting vitality for decades to come.
How do I know if it’s time to seek care?
Perimenopause and menopause are natural transitions—but that does not mean you are meant to simply endure their effects. Many women can benefit from professional care.
If changes in your sleep, mood, focus, energy, weight, or sense of well-being are interfering with your daily life, it may be time to seek support. Symptoms that are persistent, disruptive, or progressively worsening are not “just aging”—they are signals that your body is adapting to a new hormonal environment.
Not every woman needs hormone therapy. But many women benefit significantly when symptoms are thoughtfully evaluated and addressed from a menopause-trained provider. Treatment decisions are individualized and guided by:
How your symptoms are affecting your quality of life
Your personal and family health history
Your cardiovascular, metabolic, and bone health risk profile
Your goals for midlife and long-term vitality
At Radiant Health for Women, we do not treat lab numbers in isolation. Hormone testing can offer helpful context, but your lived experience matters most. Care is grounded in evidence-based guidelines and shared decision-making, tailored to your unique presentation.
You know your body. If something feels different, unsettled, or unlike you, it is worth exploring. Seeking clarity is not overreacting—it is a proactive step toward feeling like yourself again.
What does treatment look like?
Treatment during perimenopause and menopause is highly individualized. Some women benefit from hormone therapy. Others improve with non-hormonal strategies. Many need a combination of both. The right plan depends on your symptoms, medical history, risk profile, and personal goals.
Hormone Therapy - (estrogen, progesterone, and in some cases testosterone) can be safe and effective for certain women who qualify. When prescribed carefully and monitored appropriately this therapy can significantly improve quality of life by helping with many midlife health concerns:
Hot flashes and night sweats
Sleep quality and energy
Mood and cognitive clarity
Vaginal comfort and sexual health
Bone density
Cardiovascular health when started at the appropriate time
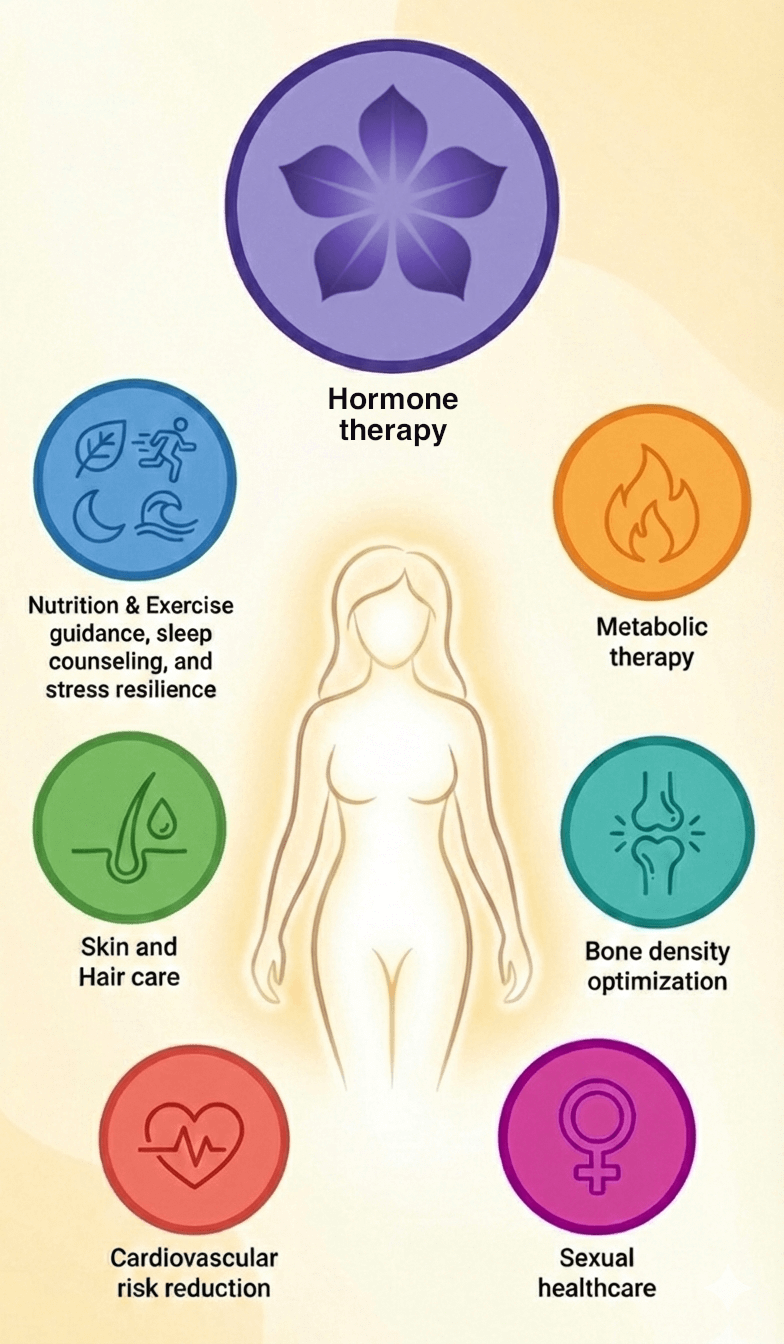
Beyond Hormones: A Whole-Body Approach - Hormone therapy is not necessary for every woman, as there are many other therapies targeted to midlife health concerns. At Radiant Health for Women, we also address:
Metabolic health, weight loss and body composition
Bone strength and osteoporosis prevention
Sexual health and intimacy concerns
Cardiovascular risk reduction
Skin and Hair changes
Nutrition and Exercise guidance, Sleep counseling, and Stress resilience
These systems are interconnected. Supporting muscle mass improves metabolic health. Improving sleep supports mood and cardiovascular function. Strengthening bones protects long-term mobility. Care is most effective when addressing the whole body.
What should I look for in a provider?

Perimenopause and menopause are complex, whole-body transitions. Symptoms vary widely from woman to woman and evolve over time. Choosing the right provider can make the difference between feeling dismissed—and feeling truly supported.
Qualifications and Training: The provider should have a formal menopause-specific certification, such as with The Menopause Society. Furthermore, a commitment to ongoing education is essential, as menopause care continues to evolve. In a 2019 survey of U.S. residents in family medicine, internal medicine, and obstetrics and gynecology, only 6.8% reported feeling adequately prepared to manage women experiencing menopause.
Care Model and Approach: The provider should offer holistic, individualized care tailored specifically to your risk profile, symptoms, and preferences. Care should address not only symptom management but also screening for chronic diseases and long-term health optimization. A good care model will offer ample time for visits and ongoing provider access to address your concerns. The model should emphasize shared decision-making to help you to make informed choices about your treatment. For complex cases the provider should collaborate with or refer to appropriate specialists.
Qualities and Characteristics: Seek a provider who listens with empathy, validates your experiences, and demonstrates cultural sensitivity. They should be willing to discuss the full range of treatment options, including both pharmacologic therapies (like hormone therapy) and non-pharmacologic approaches (such as cognitive behavioral therapy, lifestyle modifications, and behavioral strategies). The provider should offer unbiased, accurate information created without commercial influence or hidden agendas to sell products or services.
Counseling and Communication: The provider should clearly explain the risks and benefits of all therapies. They should proactively screen for mental health concerns, sexual health issues, and chronic disease risk factors such as cardiovascular disease, diabetes, and osteoporosis. They should normalize menopause as a natural transition while acknowledging when symptoms significantly affect function and quality of life.
Ultimately, the right provider will empower you with knowledge, validate your concerns, and partner with you to optimize both your current quality of life and your long-term health during this critical window of opportunity.
